Pelvic Floor Disorders
Pelvic floor disorders occur when the muscles and connective tissues supporting
the bladder, uterus, and rectum become weak or damaged. These conditions can lead
to urinary problems, bowel issues, and pelvic discomfort. Early diagnosis and
appropriate treatment help restore pelvic function and improve quality of life.
What Are Pelvic Floor Disorders?
Pelvic floor disorders involve weakening or dysfunction of the pelvic floor muscles,
which support pelvic organs. When these muscles fail to function properly,
patients may experience urinary, bowel, or pelvic symptoms.
Common Symptoms:
- Urinary or fecal incontinence
- Pelvic pressure or heaviness
- Difficulty emptying bladder or bowels
- Pain or discomfort in the pelvic region
- Bulge or prolapse felt in the vaginal or rectal area
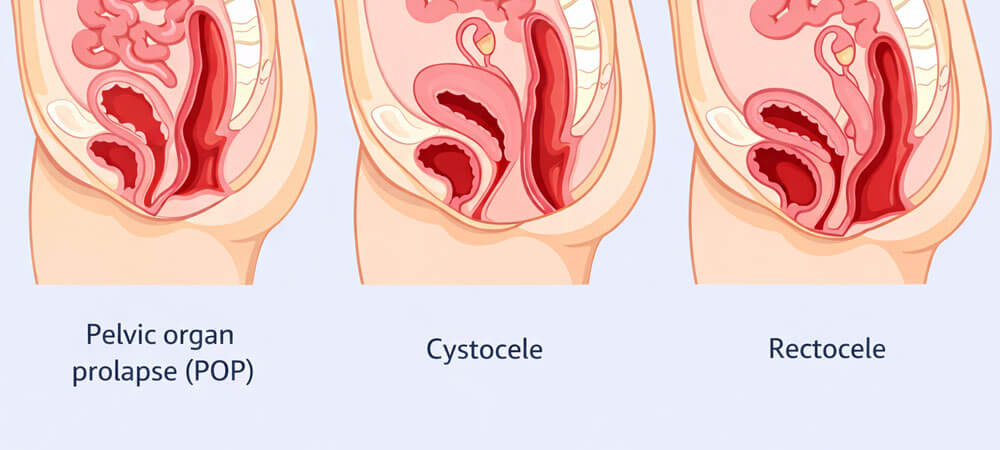
Types of Pelvic Floor Disorders:
-
Pelvic organ prolapse: Organs descend due to weakened pelvic support.
May affect bladder, uterus, or rectum.
-
Urinary incontinence: Loss of bladder control due to muscle weakness.
Common after childbirth or aging.
-
Fecal incontinence: Inability to control bowel movements.
Occurs due to muscle or nerve damage.
-
Pelvic pain disorders: Chronic pelvic pain from muscle tension or dysfunction.
Requires specialized evaluation.
Causes of Pelvic Floor Disorders:
-
Pregnancy and childbirth: Stretching and injury weaken pelvic muscles.
This is a leading cause in women.
-
Aging: Natural muscle weakening occurs with age.
Increases risk of pelvic dysfunction.
-
Chronic straining: Constipation or heavy lifting puts pressure on pelvic muscles.
Leads to long-term damage.
-
Pelvic surgeries: Prior surgeries may affect muscle and nerve support.
Contributes to pelvic floor weakness.
Prevention & Lifestyle Management:
- Perform pelvic floor (Kegel) exercises regularly
- Avoid heavy lifting and excessive straining
- Maintain healthy bowel habits
- Maintain a healthy body weight
- Seek early treatment for urinary or bowel symptoms
Treatments for Pelvic Floor Disorders:
-
Pelvic floor physiotherapy: Strengthens muscles and improves coordination.
First-line treatment for many patients.
-
Medications: Used to manage associated bladder or bowel symptoms.
Helps improve daily comfort.
-
Support devices: Pessaries provide support for prolapsed organs.
Suitable for selected patients.
-
Minimally invasive procedures: Advanced techniques restore pelvic support.
Offer faster recovery and minimal discomfort.
-
Surgical treatment: Recommended for severe or persistent pelvic floor disorders.
Restores normal pelvic anatomy and function.